|
Imagine you’re on a highway. An accident causes traffic to pile up ahead. Emergency crews redirect cars around the congestion. Finally, you’re able to get back on the road and the route is clear.
If you need heart bypass surgery, the procedure is pretty similar. A surgeon takes blood vessels from another part of your body to go around, or bypass, a blocked artery. The result is that more blood and oxygen can flow to your heart again. It can help lower your risk for a heart attack and other problems. Once you recover, you’ll feel better and be able to get back to your regular activities. Bypass surgery is also known as coronary artery bypass grafting (CABG). It’s the most common type of open-heart surgery in the U.S. Most people have great results and live symptom-free for a decade or more. Why Do I Need It? Bypass surgery treats symptoms of coronary heart disease. That happens when a waxy substance called plaque builds up inside the arteries in your heart and blocks blood and oxygen from reaching it. You may feel things like:
Coronary heart disease can lead to aheart attack. It can cause a blood clotto form and cut off blood flow. Bypass surgery can give your ticker a big health boost. How Does It Work? A surgeon removes a blood vessel, called a graft, from another part of your body, like your chest, leg, or arm. He attaches one end of it to your aorta, a large artery that comes out of your heart. Then, he attaches the other end to an artery below the blockage. The graft creates a new route for blood to travel to your ticker. If you have multiple blockages, your surgeon may do one or more bypass procedures during the same surgery. You’ll be asleep the whole time, about 3 to 6 hours on average. What Happens After Surgery? You’ll wake up in an intensive care unit (ICU). You’ll have a tube in your mouth to help you breathe. You won’t be able to talk and will feel uncomfortable. Nurses will be there to help you. They’ll remove the tube after a few hours, when you can breathe on your own. You’ll also be hooked up to machines that monitor your vital signs, like your heart rate and blood pressure, around the clock. You’ll stay in the ICU for a few days before being moved to a hospital room. You’ll stay there for about 3 to 5 days before you go home. What Will the Recovery Be Like? It’s a gradual process. You may feel worse right after surgery than you did before. This is normal. Your body needs time to recover, but you’ll feel better each day. You won’t be fully healed for about 2 months. Be sure to follow your doctor’s instructions. You may not be able to drive for 3 to 8 weeks. You’ll visit your doctor several times during the first few months to track your progress. Call him if your symptoms don’t improve or you’re feeling worse. What Are the Risks? All surgeries come with the chance of problems. Some of the possible ones include:
Once you’ve recovered, your symptoms of angina will be gone or much better. You’ll be able to be more active, and you’ll have a lower risk of getting a heart attack. Best of all, the surgery can add years to your life. Read Entire Article: http://www.webmd.com/heart-disease/guide/heart-disease-bypass-surgery#1 By Rob Lamberts, MD,
It’s 2 AM and you wake up with chest pain, aka angina. What should you do? Maybe it’s just indigestion, but maybe it’s a heart attack. How do you know what to do? When Is Chest Pain Serious? Heart disease kill more people in the U.S. than any other single disease, and the main symptom that people have from a heart attack is chest pain. It’s also the leading cause of death in women in the US, according to the Centers for Disease Control and Prevention. But the term chest pain is actually misleading. Heart pain is not always described as being painful, and it’s not always in the chest. For that reason, I like the Latin term angina pectoris, which means “sensation in the chest.” This is not just a vocabulary lesson; people die because what they are feeling isn’t actually chest pain and so they stay at home and have a heart attack. Today I’ll focus on the symptom that brings people into my office, and then over the next few weeks I’ll cover the cause and the treatment of heart disease. When Is Chest Pain a Heart Attack? So how can you tell if you should worry with your angina symptoms? There are two main factors that help me decide when to worry: the details of the actual symptoms, and the patient's risk factors for heart disease. The typical symptoms of angina are described as:
What Are Other Symptoms of a Heart Attack? Those are the typical symptoms, and the presence of all of the above descriptions certainly is cause for worry. But many people have other atypical symptoms that may still be a cause for concern. These atypical symptoms of heart attacks are especially common in women, according to a study in the Journal of the American Medical Association. Here are some of the other symptoms and misconceptions about heart attack signs: Pain isn’t on the left side: Sometimes the pain is not on the left, but on the right, the center, or even at the top of the abdomen. Absence of pain: Some people have no pain at all; instead they just have shortness of breath. Some patients, particularly diabetics, can have no symptoms at all. One-half of the people having heart attacks didn’t even notice it. Varied quality of pain: Some experience a sharp, burning, gassy pain, or a feeling of indigestion. I also had one patient describe his symptoms as “a cold feeling in the chest” whenever he breathed. How Long Does Chest Pain Related to a Heart Attack Last? Aside from what the chest pain feels like, you should also pay attention to how long the pain lasts. Chest pain related to a heart attack doesn’t typically last just a few seconds. Heart chest pain almost always lasts at least 5 minutes, and doesn’t typically last more than 20 to 30 minutes continuously. Pain that comes on after exercise or exertion but consistently goes away with rest may represent a narrowing of the blood vessels that supply blood to the heart. That could lead to a heart attack eventually, but it isn’t always an emergency, either. However, it is vital that you discuss these symptoms with your doctor right away.. What are the Risk Factors for a Heart Attack?The other major things to consider when determining whether your chest pain is a heart-related emergency are your risk factors. It’s a big difference when a 20-year-old woman comes in with chest pain than when a 50-year-old male diabetic who smokes comes in. The risk factors for heart attacks include: Age – risk for heart attacks begins to rise for men at age 40 and women at 50. It can still happen below that age, but it’s a lot less likely. Sex – men are at higher risk than women, although the disease still kills a huge number of women each year. Genetics – if a member of your immediate family (parent or sibling) has coronary heart disease, your risk is substantially higher. That risk is especially high if that family member is a man under 55 or a woman under 65 Smoking – people often think of smoking as a danger to the lungs (which it is), but the biggest risk of death from smoking is from heart attacks. I recommend my patients quit smoking and take up something safer, like tightrope walking, javelin catching, or training pit bulls. Using the results of the revolutionary large Framingham Study, you can calculate your own risk of developing cardiovascular disease in the next 10 years using their interactive calculator online. This is a tool that some physicians often use to determine a patient’s risk. Hypertension and diabetes – Having these diseases also increase risk for heart attack. High cholesterol – this is a complex subject, so please refer to my article on cholesterol to get an accurate picture. If you need helpinterpreting your cholesterol, or tips on how to lower it, we’ve covered those topics, too. The more of these risk factors you personally have, the more seriously you should take any chest pain you experience. I will often be more concerned about a high-risk person with atypical symptoms than a low-risk person with classic symptoms. When Is Chest Pain NOT a Heart Attack?There are some symptoms that reassure me the chest pain isn’t related to the heart: Pain that persists for hours – heart chest pain will either go away after 20-30 minutes, or will end up in a heart attack. Pain that gets worse with movement – or pain that gets worse when you press on that area of the chest is probably from the muscles or the bones in the chest, not the heart. Pain that you can point to with a single finger – heart pain tends to be hard to pinpoint. Pain that is triggered with breathing in – very brief, sharp pain that occurs with taking a deep breath is a typical presentation of pleuritis, inflammation of the lining of the lungs. I hope these tips help you. Learn the symptoms of heart pain and know your risk factors. If you are experiencing an acute chest pain more consistent with heart symptoms and/or have atypical symptoms and risk factors for heart disease, get to the emergency room immediately, even if you have to call an ambulance. If you are high risk and have classic symptoms, get to the emergency room immediately, even if you have to call an ambulance. Remember: it’s always OK to get things checked out. It’s far better to be seen for symptoms that are not serious than to stay home with serious symptoms. Let me remind you that this is for informational purposes only. My goal is to add to your medical knowledge and translate some of the weird medical stuff you hear, so when you do go to your doctor, your visits will be more fruitful. I don’t intend to replace your doctor; he or she is the one you should always consult about your own medical condition. Read Article: http://www.quickanddirtytips.com/health-fitness/prevention/when-is-chest-pain-serious If you or someone you love needs emergency heart treatment, it’ll help to know when they should get to the emergency room and what to expect.
It's also important to know how you can be prepared. When to Go to the ER For many people, knowing when to seek emergency care isn't always clear. Most people know to call 911 right away when faced with a life-threatening situation, such as loss of consciousness, breathingtrouble, or serious trauma. But heart attack symptoms aren't always as clear. It may be hard to tell if they’re from a heart crisis or heartburn, for example. Remember, it’s always better to be safe than sorry. If you feel it’s an emergency, call 911 and ask them to send an ambulance right away. EMS personnel can start caring for you or your loved one immediately, and they’ll alert the emergency room to let them know you are coming. If you have these symptoms, go to the emergency room immediately:
Be Prepared You never know when you may need to go to the emergency room, so it's best to be ready. Here are some steps you can take now to make any visit to the emergency room easier: Create a file -- and update it regularly -- that includes:
Keep this file in a place where you can find it quickly. Check your health insurance to find out which hospital emergency rooms your plan covers. Keep a list of their names, addresses, and phone numbers. But if you think you are having a heart attack, call 911. Don’t drive yourself, and don’t have someone else drive you. What to Bring
If there’s time, have a loved one let your doctor know what’s going on. What to Expect When You Arrive Emergency rooms treat the most serious illnesses first. If you arrive with symptoms of a heart attack, they’ll see you quickly. Doctors will work to confirm your diagnosis, relieve your symptoms, and treat the problem. Depending upon your symptoms, you may have one or more of the following:
Be prepared to answer a lot of questions, including ones about:
Transfer from Emergency Room to Hospital Room Not everyone who goes to the emergency room with chest pain is admitted to the hospital. But if there’s a reasonable chance that the pain is due to a heart attack or other serious condition, you will be. For the first 24 hours after a heart attack, you’re usually in a coronary care unit (CCU) or an intensive care unit (ICU). There, skilled staff will closely check your heart. A series of electrocardiograms and blood tests will be performed. Doctors will continue to keep close watch over you and give you meds as needed. Your doctor may ask for more tests. If you’re stable after 24 hours in the CCU or ICU, you may be moved to the "telemetry" floor, where a cardiac care team will continue to care for you. Depending upon the severity of the heart attack and how quickly you received treatment, you may be able to go home in 2 to 4 days. When You Get Home From the Hospital
Read Entire Article: http://www.webmd.com/heart-disease/what-to-expect-in-the-er#1 If something went wrong with your heart, would you know it?
Not all heart problems come with clear warning signs. There is not always an alarming chest clutch followed by a fall to the floor like you see in movies. Some heart symptoms don’t even happen in your chest, and it’s not always easy to tell what’s going on. "If you're not sure, get it checked out," says Charles Chambers, MD, director of the Cardiac Catheterization Laboratory at Penn State Hershey Heart and Vascular Institute. That’s especially true if you are 60 or older, are overweight, or have diabetes, high cholesterol, or high blood pressure, says Vincent Bufalino, MD, an American Heart Association spokesman. "The more risk factors you have," he says, "the more you should be concerned about anything that might be heart-related." Especially watch out for these problems: 1. Chest Discomfort It’s the most common sign of heart danger. If you have a blocked artery or are having a heart attack, you may feel pain, tightness, or pressure in your chest. "Everyone has a different word for that feeling," Chambers says. "Some people say it's like an elephant is sitting on them. Other people say it's like a pinching or burning." The feeling usually lasts longer than a few minutes. It may happen when you're at rest or when you're doing something physical. If it's just a very brief pain -- or if it's a spot that hurts more when you touch or push on it -- it's probably not your heart, Chambers says. You should still get it checked out by a doctor. If the symptoms are more severe and don’t go away after a few minutes, you should call 911. Also, keep in mind you can have heart problems -- even a heart attack -- without chest pain. That’s particularly common among women. 2. Nausea, Indigestion, Heartburn, or Stomach Pain Some people have these symptoms during a heart attack. They may even vomit, Chambers says. Women are more likely to report this type of symptom than men are. Of course, you can have an upset stomach for many reasons that have nothing to do with your heart. It could just be something you ate, after all. But you need to be aware that it can also happen during a heart attack. So if you feel this way and you’re at risk for heart problems, let a doctor find out what’s going on, especially if you also have any of the other symptoms on this list. 3. Pain that Spreads to the Arm Another classic heart attack symptom is pain that radiates down the left side of the body. "It almost always starts from the chest and moves outward," Chambers says. "But I have had some patients who have mainly arm pain that turned out to be heart attacks." 4. You Feel Dizzy or Lightheaded A lot of things can make you lose your balance or feel faint for a moment. Maybe you didn’t have enough to eat or drink, or you stood up too fast. But if you suddenly feel unsteady and you also have chest discomfort or shortness of breath, call a doctor right away. "It could mean your blood pressure has dropped because your heart isn't able to pump the way it should," Bufalino says. 5. Throat or Jaw Pain By itself, throat or jaw pain probably isn't heart related. More likely, it's caused by a muscular issue, a cold, or a sinus problem. But if you have pain or pressure in the center of your chest that spreads up into your throat or jaw, it could be a sign of a heart attack. Call 911 and seek medical attention to make sure everything is all right. 6. You Get Exhausted Easily If you suddenly feel fatigued or winded after doing something you had no problem doing in the past -- like climbing the stairs or carrying groceries from the car -- make an appointment with your doctor right away. "These types of significant changes are more important to us than every little ache and pain you might be feeling," Bufalino says. Extreme exhaustion or unexplained weakness, sometimes for days at a time, can be a symptom of a heart attack, especially for women. 7. Snoring It’s normal to snore a little while you snooze. But unusually loud snoring that sounds like a gasping or choking can be a sign of sleep apnea. That’s when you stop breathing for brief moments several times at night while you are still sleeping. This puts extra stress on your heart. Your doctor can check whether you need a sleep study to see if you have this condition. If you do, you may need a CPAP machine to smooth out your breathing while you sleep. 8. Sweating Breaking out in a cold sweat for no obvious reason could signal a heart attack. If this happens along with any of these other symptoms, call 911 to get to a hospital right away. Don’t try to drive yourself. 9. A Cough That Won’t Quit In most cases, this isn't a sign of heart trouble. But if you have heart disease or know you're at risk, pay special attention to the possibility. If you have a long-lasting cough that produces a white or pink mucus, it could be a sign of heart failure. This happens when the heart can't keep up with the body's demands, causing blood to leak back into the lungs. Ask your doctor to check on what’s causing your cough. 10. Your Legs, Feet, and Ankles Are Swollen This could be a sign that your heart doesn’t pump blood as effectively as it should. When the heart can't pump fast enough, blood backs up in the veins and causes bloating. Heart failure can also make it harder for the kidneys to remove extra water and sodium from the body, which can lead to bloating. 11. Irregular Heart Beat It's normal for your heart to race when you are nervous or excited or to skip or add a beat once in a while. But if you feel like your heart is beating out of time for more than just a few seconds, or if it happens often, tell your doctor. "In most cases, it's caused by something that's easy to fix, like too much caffeine or not enough sleep," Bufalino says. But occasionally, it could signal a condition called atrial fibrillation that needs treatment. So ask your doctor to check it out. Read Entire Article: http://www.webmd.com/heart-disease/features/never-ignore-symptoms#3 If you care about heart health (and really, who doesn't?), you better sit down. The so-called "good" cholesterol, HDL, may not be so great for your health after all.
A large new study of people in the general population found that those who have the highest HDL cholesterol aren't less likely to have heart attacks or strokes; and that while people with low levels of HDL are more likely to have those health troubles, it’s likely due to lifestyle habits and other risk factors. The study, released Monday in the Journal of the American College of Cardiology, tracked more than 631,000 Canadians, ages 40 and up, for about five years. The findings are surprising, since it was thought that boosting HDL levels in addition to lowering “bad” LDL was best for a healthy heart and plaque-free arteries. HDL, which stands for high-density lipoprotein, is a fat-carrying protein known to ferry cholesterol out of artery walls. But this isn’t the first time doubt has been cast on the idea of HDL as “good” cholesterol. In August, a study on 1.7 million U.S. veterans also found that people with high HDL had increased rates of death from all causes. Meanwhile, clinical trials for drugs that raise HDL have failed to significantly improve health for participants. Now, these studies may hold a clue as to why. The researchers found that low levels of HDL were bad (which was known), but that the highest levels were bad for your health too—which is new. People in the study with low HDL tended to be obese, to smoke, and to have poor diet and exercise habits. And they were more likely to have low incomes, and high triglycerides (another important aspect of total cholesterol). Compared to people with HDL in the middle range, those with low levels (less than 50 mg/dl in women and less than 40 mg/dl in men) were more likely to die over the course of the study. That was true for heart- or stroke-related deaths and other causes, such as cancer. These link remained even after the authors controlled for unhealthy lifestyle factors, although the authors say they couldn't factor out every potential contributor. (Most experts recommend an HDL level over 40 mg/dL and "the higher, the better.") The biggest surprise came when they looked at people with high HDL. The risk of heart- or stroke-related death didn’t drop for people with the highest HDL levels versus those in the middle. And those with the highest HDL levels (greater than 70 mg/dl in men and greater than 90 mg/dl in women) actually had an increased risk of death from non-heart or stroke-related causes. The reason for this increased risk is unknown, the authors say. Previous research suggests that alcohol could play a role, but here, the link remained even after the researchers controlled for heavy drinking. Overall, the authors concluded that HDL may not be the best measure of heart disease risk—and that interventions to raise HDL may not, in fact, reduce that risk as once hoped. Rather, their findings suggest that HDL “is a marker of poor general health" and changing the number itself, say with medication, may not make any difference. "The link between good cholesterol and heart disease is complex,” said lead author Dennis T. Ko, MD, associate professor at the Institute for Clinical Evaluative Sciences in Toronto, in a press release. “But it seems certain that there is a connection between people with low good cholesterol levels and other well-known risk factors for heart disease such as poor diet and exercise habits and other medical conditions." "Focusing on raising HDL is likely not going to help these patients,” he added, “but these findings show that one of the best interventions in treating and preventing heart disease continues to be lifestyle changes." So, instead of achieving a specific HDL, you should focus on quitting smoking, exercising and having a healthy weight—all factors with ironclad evidence that they help your heart. The authors acknowledge that their study had limitations, including an inability to look at different subclasses and particle sizes of HDL molecules. An editorial published with the study agrees that further research in these areas could potentially show new ways in which HDL actually does relate to heart disease. Read Article: https://www.yahoo.com/beauty/good-cholesterol-may-not-heart-185857387.html The signs and symptoms of coronary heart disease (CHD) may differ between women and men. Some women who have CHD have no signs or symptoms. This is called silent CHD.
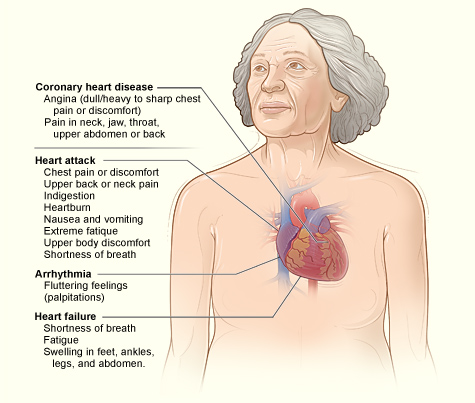
Silent CHD may not be diagnosed until a woman has signs and symptoms of a heart attack, heart failure, or an arrhythmia (irregular heartbeat). Other women who have CHD will have signs and symptoms of the disease. A common symptom of CHD is angina. Angina is chest pain or discomfort that occurs when your heart muscle doesn't get enough oxygen-rich blood. In men, angina often feels like pressure or squeezing in the chest. This feeling may extend to the arms. Women can also have these angina symptoms. But women also tend to describe a sharp, burning chest pain. Women are more likely to have pain in the neck, jaw, throat, abdomen, or back. In men, angina tends to worsen with physical activity and go away with rest. Women are more likely than men to have angina while they're resting or sleeping. In women who have coronary microvascular disease, angina often occurs during routine daily activities, such as shopping or cooking, rather than while exercising. Mental stress also is more likely to trigger angina pain in women than in men. The severity of angina varies. The pain may get worse or occur more often as the buildup of plaque continues to narrow the coronary (heart) arteries. Signs and Symptoms Coronary Heart Disease Complications Heart Attack The most common heart attack symptom in men and women is chest pain or discomfort. However, only half of women who have heart attacks have chest pain. Women are more likely than men to report back or neck pain, indigestion, heartburn, nausea (feeling sick to the stomach), vomiting, extreme fatigue (tiredness), or problems breathing. Heart attacks also can cause upper body discomfort in one or both arms, the back, neck, jaw, or upper part of the stomach. Other heart attack symptoms are light-headedness and dizziness, which occur more often in women than men. Men are more likely than women to break out in a cold sweat and to report pain in the left arm during a heart attack. Heart Failure Heart failure is a condition in which your heart can't pump enough blood to meet your body's needs. Heart failure doesn't mean that your heart has stopped or is about to stop working. It means that your heart can't cope with the demands of everyday activities. Heart failure causes shortness of breath and fatigue that tends to increase with physical exertion. Heart failure also can cause swelling in the feet, ankles, legs, abdomen, and veins in the neck. Arrhythmia An arrhythmia is a problem with the rate or rhythm of the heartbeat. During an arrhythmia, the heart can beat too fast, too slow, or with an irregular rhythm. Some people describe arrhythmias as fluttering or thumping feelings or skipped beats in their chests. These feelings are called palpitations. Some arrhythmias can cause your heart to suddenly stop beating. This condition is called sudden cardiac arrest (SCA). SCA causes loss of consciousness and death if it's not treated right away. Signs and Symptoms of Broken Heart Syndrome The most common signs and symptoms of broken heart syndrome are chest pain and shortness of breath. In this disorder, these symptoms tend to occur suddenly in people who have no history of heart disease. Arrhythmias or cardiogenic shock also may occur. Cardiogenic shock is a condition in which a suddenly weakened heart isn't able to pump enough blood to meet the body's needs. Some of the signs and symptoms of broken heart syndrome differ from those of heart attack. For example, in people who have broken heart syndrome:
Read Entire Article: https://www.nhlbi.nih.gov/health/health-topics/topics/hdw/signs We always associate chest pain with heart attacks, and for good reason, but it’s not the whole story — especially for women. While chest pain is the most common symptom of a heart attack, women can have symptoms that aren’t related to chest pain at all. They need to be on the lookout for other, subtler symptoms. Also, we need to dig deeper into the symptom of chest pain for both men and women as it relates to heart attacks. It is seldom as dramatic as you might think, and it can feel like pressure or heart burn that comes on over time. Below, find three symptoms you should watch for, including information about how to tell if they are benign or cause for concern. 1. Unusual fatigue Like many women, you’re probably busy most of the time. You may take care of a family, run a household, work outside the home and care for aging parents. You are probably also tired a lot of the time. Most likely this is normal. But you should pay attention to fatigue if it is new or dramatic. Here’s what to watch out for:
2. Sweating and/or shortness of breath As women age, a lack of exercise and gradual weight gain cause issues like shortness of breath. Hot flashes are a common complaint for many women during menopause. But these symptoms can signal a heart problem when they happen in certain situations:
3. Neck, jaw, back pain As intricate as our body’s systems are, they are very adept at giving signals when there is something wrong. When there is a problem with the heart, it triggers nerves in that area, but you sometimes feel pain elsewhere. Pain in the jaw, back or arms may signal a heart condition, especially if the origin is hard to pinpoint (for example there is no specific muscle or joint that aches). Also, if the discomfort begins or worsens when you are exerting yourself, and then stops when you quit exercising, you should get it checked out. Here are some other signs to look out for:
What to do if you notice symptoms Women often say they noticed some of these three warning signs weeks or a month before a heart attack. The sooner you report a problem, the better the chances are of catching an issue before it becomes a full-blown heart attack. If you experience any of these symptoms, take note and visit your doctor as quickly as possible. When you see your doctor:
Your doctor likely will listen to your symptoms and check your pulse and blood pressure. He or she may order blood work, which will show whether your heart is damaged. Your doctor also may use an electrocardiogram (echo) to tell whether the electrical activity of your heart is normal, or an echocardiogram (EKG) to view images of the heart to see if damage has occurred. All this is important in identifying any problems and taking steps to intervene before a possible heart attack. When to call 9-1-1 Get help right away if you have chest pain or discomfort along with any of these symptoms, especially if they last longer than five minutes:
Read Article: https://health.clevelandclinic.org/2016/03/women-dont-ignore-3-subtle-heart-attack-symptoms/ Doctors writing in the journal BMJ Case Reports describe the case of a healthy 55-year-old man in India who developed serious heart problems several weeks after being attacked by a swarm of bees.
While walking in a forest, he suffered more than 50 stings, and he was admitted to hospital with facial puffiness, breathlessness and sudden tiredness. He had no history of heart problems and heart tests were normal. After initial treatment, his condition improved and he was discharged with anti-inflammatory medication. But around three weeks later, he was back in hospital after developing a dangerously slow heart rate, repeated fainting, and suffering acardiac arrest. He almost died. The doctors managed to save his life by inserting a temporary pacemaker, which was later replaced with a permanent pacemaker. His condition improved and he was eventually discharged home. The doctors suspect the man had developed Kounis syndrome (a group of acute coronary events) triggered by a delayed allergic reaction to the massive amount of bee venom in his system. Another possible reason, they say, could have been that the bees had consumed the nectar of a rhododendron flower, which contains ‘grayanotoxin’ (a natural sodium channel blocker that can slow the heart). The cardiac effects of bee venom have been previously reported. But this case is of particular importance, explain the authors, “because earlier accounts of massive bee stings have not reported significant bradycardia. Hence, we were unaware of this complication, and hesitated to implant a temporary pacemaker.” This report highlights the need to consider heart complications in patients with multiple bee stings, and the need for urgent action in order to prevent death, they conclude. Case report: Possible complication of bee stings and a review of the cardiac effects of bee stings http://casereports.bmj.com/content/2016/bcr-2016-213974 Read Article: http://medicalxpress.com/news/2016-11-doctors-prolonged-heart-effects-multiple.html Facebook:
https://www.facebook.com/johnpaul.runyon Twitter: https://twitter.com/johnpaulrunyon Wordpress: https://drjohnpaulrunyon.wordpress.com/ Tumblr: http://drjohnpaulrunyon.tumblr.com/ Weebly: http://johnpaulrunyon.weebly.com/ Websites: JohnPaulRunyon.com JohnPaulRunyon.org JohnPaulRunyon.net John-Paul-Runyon.com JohnPaulRunyonInfo.com |
Archives
May 2017
Categories |



 RSS Feed
RSS Feed
